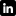By Dr Alex Mercer
Most commentary on a national aids control council starts with the wrong premise. It assumes the term describes a standard institution that every country should already have. It doesn’t. In the UK, there is no body formally called a National AIDS Control Council. That absence isn’t a semantic footnote. It’s the starting point for a more useful policy question: which governance functions matter most, and how can countries build them even when they use different institutional labels?
For G7 and G20 governments, that question is more important than institutional mimicry. The strongest HIV responses don’t succeed because a council exists on paper. They succeed when governments create a coordinating authority that can align strategy, finance, delivery, and accountability across ministries, donors, clinicians, and community organisations. That’s the transferable lesson from national models often discussed under the banner of a national aids control council.
The UK case sharpens the point. Search results don’t identify a UK equivalent under that name, though the UK Health Security Agency and wider HIV surveillance and commissioning frameworks perform some adjacent functions. Comparative analysis therefore matters. Kenya’s council model, and India’s organisational approach, show how countries can use a central coordinating mechanism to reduce fragmentation, improve implementation discipline, and direct resources towards populations that ordinary health-system planning often underserves.
For a global policy audience, the value of studying these models isn’t descriptive. It’s operational. A well-designed national AIDS coordinating body offers a template for broader health governance, especially for syndemics that cut across HIV, TB, viral hepatitis, migration, homelessness, and prison health. The key lesson isn’t that every state needs the same institution. It’s that every state needs the same core capacities.
Table of Contents
- Introduction The Global Health Governance Model
- Understanding The Core Mandate And Principles
- Governance And Multi-Sectoral Coordination
- Strategic Planning And Sustainable Financing
- Comparative Lessons from Global Case Studies
- Current Challenges And Unaddressed Policy Gaps
- Actionable Recommendations For G7 and G20 Policymakers
Introduction The Global Health Governance Model
A national aids control council is best understood as a governance model before it is understood as an institution. In many countries, HIV policy failed when health ministries tried to manage it as a narrow clinical programme. HIV touches education, labour, migration, prisons, social protection, procurement, and fiscal planning. That makes coordination a state capacity issue, not just a medical one.
This is why the council model has remained relevant. It gives one authority responsibility for convening actors that otherwise operate on separate mandates, budgets, and reporting lines. In low-prevalence and high-income settings, governments often assume those coordinating functions can stay dispersed because the health system is mature. That assumption often hides fragmentation rather than solving it.
The comparative record suggests that the institutional name matters less than the architecture behind it. India’s National AIDS Control Organisation is one example of a national coordinating approach embedded under the Ministry of Health. Kenya’s model demonstrates a stronger council-style mechanism with explicit attention to cross-sector implementation, community engagement, and unified monitoring. Neither model is a plug-and-play export. Both show that political authority, clear strategy, and operational discipline have to sit together.
A country doesn’t need the same acronym as Kenya or India. It needs a mechanism with enough authority to align incentives across the system.
For G20 policymakers, that lesson reaches beyond HIV. The same machinery can support TB integration, viral hepatitis strategy, and responses to overlapping vulnerability among migrants, homeless populations, and people in custody. HIV governance has long served as an early laboratory for whole-of-government health policy. Countries that ignore that experience usually end up relearning the same coordination problems at higher cost.
Understanding The Core Mandate And Principles

The defining mandate of a national aids control council is to make a national HIV response coherent. That sounds obvious, but coherence is rarely automatic. Health ministries commission treatment. Finance ministries control fiscal space. Interior ministries shape prison health. Education ministries influence prevention environments. Community organisations often know more about barriers to access than any central agency. Without a coordinating authority, each actor can perform well inside its own silo while the national response underperforms.
The mandate is coordination, not duplication
A capable council doesn’t replace service providers. It sets direction, aligns incentives, and imposes a common logic on delivery. In practice, that means several functions:
- Strategy setting: One national framework prevents agencies from funding competing priorities.
- Convening power: Senior leadership can bring ministries, donors, civil society, and implementing partners into the same decision space.
- Monitoring and evaluation: A common results framework makes it harder for parallel programmes to claim success on incompatible metrics.
- Course correction: Councils can identify where implementation is weakest, especially in hard-to-reach populations.
Kenya’s example is useful because it shows what happens when these functions are tied together rather than administered separately. Kenya’s National AIDS Control Council’s strategic plan adopted the Three Ones principle and linked targeted interventions for high-risk groups to a unified monitoring approach. According to the cited benchmark, that model was associated with an 18% reduction in new incidence in 2022 through a network of over 1,200 drop-in centres, illustrating how governance design can shape delivery results (Kenya and the NACO reference point).
A related policy discussion on integrated disease responses appears in this analysis of closing gaps on AIDS, tuberculosis, and malaria.
Why the Three Ones still matter
The Three Ones remain useful because they solve an enduring public-sector problem: too many plans, too many coordinators, and too many measurement systems. Even advanced health systems drift into that pattern when national strategies, local commissioners, and community providers all use different assumptions about need and performance.
A short diagnostic shows why the principle still travels well:
| Governance problem | What the council model does |
|---|---|
| Multiple plans competing for funds | Creates one agreed action framework |
| Overlapping leadership mandates | Establishes one coordinating authority |
| Fragmented reporting | Uses one monitoring and evaluation system |
Practical rule: If a country can’t say who arbitrates trade-offs across prevention, treatment, and outreach, it doesn’t yet have an effective national coordinating model.
That matters in high-income countries too. The absence of a formal national aids control council in the UK shouldn’t be read as proof that the function is unnecessary. It should be read as an invitation to ask where those functions sit now, and whether they’re strong enough to manage equity, retention, and integrated delivery.
Governance And Multi-Sectoral Coordination

The hardest part of HIV governance isn’t writing strategy. It’s making organisations with different mandates act on it. A national aids control council works when it sits high enough in government to compel cooperation, yet close enough to implementation to see where policy breaks down. That balance is difficult. Too far from frontline delivery, and the council becomes ceremonial. Too embedded in one ministry, and it loses the authority to coordinate the rest of government.
Authority determines whether coordination works
The most effective council-style bodies usually have political backing from the centre of government or a clearly authorized national ministry. That position changes behaviour. Finance officials take the process more seriously. Donors are more willing to align with national plans. Civil society has a clearer route into formal decision-making. Procurement and data systems can be reconciled rather than allowed to diverge.
The governance logic is straightforward. HIV policy requires joint decisions on issues that no single actor can settle alone, such as who gets prioritised, how community delivery is funded, and how overlapping disease burdens are managed. If those decisions are pushed down into fragmented commissioning arrangements, the system often protects incumbency instead of access.
Three coordination relationships are especially important:
- Government to government: Health, finance, justice, education, and social protection ministries need a forum where trade-offs are explicit.
- State to community: Key populations need representation that is substantive, not symbolic.
- Government to external partners: Donors and NGOs should map to national priorities rather than build parallel channels.
The broader logic of cross-government action is reflected in this discussion of health in all policies.
The council model as a transaction-reduction device
One way to understand the council model is as a way to reduce transaction costs inside the state. Without a central mechanism, each ministry negotiates separately with implementers, each donor asks for its own reporting, and each programme defines target populations in slightly different ways. That doesn’t only waste time. It weakens accountability because no single body can identify where the national response is failing.
A functional council changes that dynamic by standardising who decides what. It clarifies lines of responsibility and shortens the route from problem identification to policy response.
Good governance in HIV isn’t simply coordination for its own sake. It is coordinated authority applied to populations that fragmented systems routinely miss.
Many high-income countries overestimate their own performance. They often have strong clinics, strong epidemiology, and strong formal entitlements. Yet if responsibility for outreach, retention, and wraparound care is dispersed, vulnerable groups still fall through the gaps. Strong institutions in the plural don’t automatically create a strong system in the singular.
Strategic Planning And Sustainable Financing
The strategic value of a national aids control council becomes most visible in financing. HIV responses falter when budgeting follows administrative boundaries instead of epidemiological need. A council-style model can correct that by tying money to a national plan with clear implementation responsibilities and common performance measures.
Human resources are part of financing strategy
One of the clearest lessons from Kenya’s model is that financing isn’t only about commodities and service contracts. It’s also about implementation capability. According to Kenya’s technical support and capacity-building framework, fragmented training before the current strategic period contributed to implementation gaps of 15% to 20%. After targeted mentorship and certification programmes were introduced, coverage in key populations rose 28%, contributing to a 12% annual reduction in new infections (Kenya technical support and capacity building).
That result matters because it reframes workforce spending. Training is often treated as an overhead that can be trimmed when budgets tighten. The Kenyan evidence suggests the opposite. In a targeted HIV response, workforce quality is part of the intervention itself. If outreach workers, counsellors, and adherence staff are unevenly prepared, programme design won’t survive contact with reality.
A financing debate focused only on drugs and diagnostics will miss that point.
What sustainable financing looks like in practice
Sustainable financing has three features. It is planned, integrated, and traceable. Planned means the government uses a multi-year strategy rather than a patchwork of short projects. Integrated means community delivery, workforce development, and clinical services are costed as parts of one response. Traceable means policymakers can see whether funds reach the populations and geographies they are intended to reach.
This has direct relevance for G20 governments facing tighter budgets and more political scrutiny over value for money. The right question isn’t whether HIV financing can be cut without visible disruption in the short term. It’s whether disinvestment from coordination and targeted delivery creates higher downstream costs through late diagnosis, poor retention, or uncontrolled transmission.
A practical way to assess financing design is to ask:
- Are implementation bottlenecks costed? If not, the plan is aspirational.
- Is community delivery funded as core infrastructure? If not, the plan will underperform in marginalised populations.
- Can the system link spending to outcomes? If not, accountability will remain rhetorical.
A wider debate on resource alignment in health systems appears in this piece on financing universal health coverage.
The broader lesson is that council-style planning improves fiscal efficiency by reducing fragmentation. It doesn’t guarantee success. It does make underperformance easier to detect and harder to excuse.
Comparative Lessons from Global Case Studies
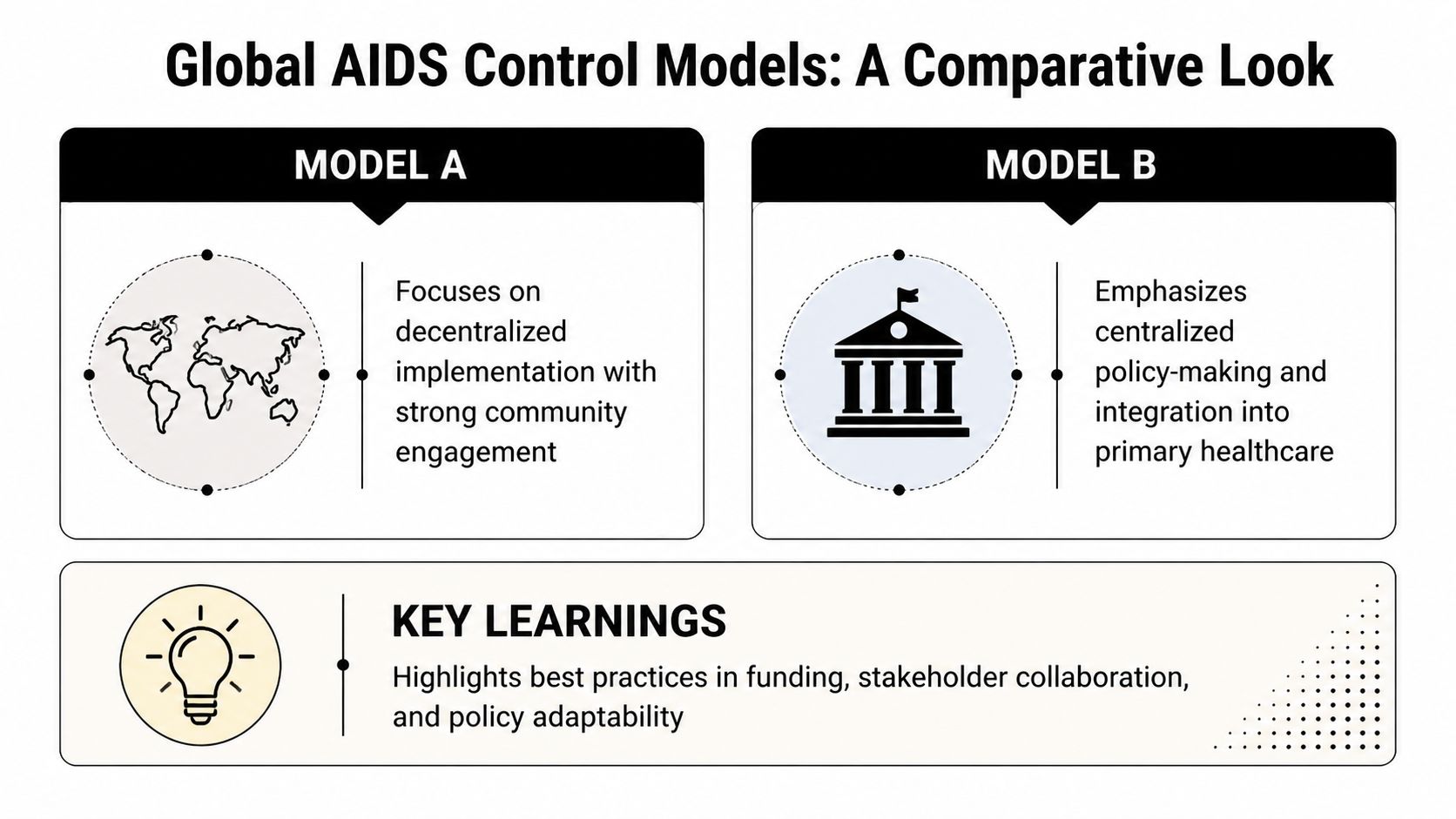
Comparative analysis is useful only when it separates form from function. Kenya and India don’t run identical systems, and they shouldn’t. Their epidemiology, administrative structures, and political settlements differ. What matters for policymakers is which design choices travel.
Kenya and India show different routes to the same objective
Kenya’s model is valuable because it makes coordination visible. Its use of the Three Ones, targeted interventions, and decentralised drop-in centre network points to a governance style that gives community-facing delivery a formal place inside national strategy. India’s model, by contrast, is often discussed as an organisational structure under the health ministry. That arrangement can support scale and policy continuity, but it raises a different design question: how much autonomy should a national HIV response retain when it is embedded in a large ministry with many competing priorities?
A simple comparison helps:
| Design feature | Kenya-style lesson | India-style lesson |
|---|---|---|
| Coordinating logic | Strong cross-sector council function | Strong programme organisation within health governance |
| Delivery emphasis | Community-facing targeted interventions | Administrative integration and national programme continuity |
| Transferable policy question | How to protect outreach and accountability | How to avoid dilution inside broader health bureaucracy |
No single approach is always superior. The right choice depends on where a country’s bottleneck sits. If the problem is fragmentation across sectors, the council model has an advantage. If the problem is long-term programme institutionalisation, an embedded national organisation may offer stability.
Equity fails first when community financing weakens
The most important comparative lesson isn’t structural. It concerns equity. Systems that look strong at the centre can still fail populations at the edge. UNAIDS reports that the share of global HIV funding channelled through communities fell from 31% in 2012 to 20% in 2021, a trend that the organisation links to widening inequities in the HIV response (UNAIDS equity in the HIV response).
That decline carries a warning for G7 and G20 governments. Community financing is often the first line item treated as flexible because it can seem administratively small and politically invisible. In reality, it often supports the services that formal institutions are least equipped to deliver well, including trust-building, navigation, peer support, and access among criminalised or stigmatised groups.
When community channels weaken, the system doesn’t become more efficient. It becomes less equitable and less truthful about where unmet need sits.
For the UK and other high-income countries, that is the hidden relevance of the national aids control council debate. The issue isn’t whether to copy another country’s institution. It’s whether domestic HIV governance gives marginalised groups a durable place in financing, planning, and accountability.
Current Challenges And Unaddressed Policy Gaps

The most misleading narrative in HIV policy is that countries with advanced health systems have largely solved the governance problem. They haven’t. They’ve often solved parts of the clinical problem while leaving major weaknesses in access, retention, and community reach.
Retention in care is the governance test high-income systems still fail
Recent evidence cited in the background materials indicates that fewer than half of people living with HIV in the UK are consistently retained in care, with weaknesses linked to distance, uneven service delivery, and insufficient mapping of underserved areas (study on HIV service access and retention challenges). That finding should change the tone of policy debate. Retention is often discussed as a behavioural issue or a service issue. It is also a governance issue.
If people disengage because services are too distant, poorly coordinated, or difficult to access, then the system has failed to organise care around real pathways of access. A council-style model can’t solve that by itself, but it does create a mechanism for integrating surveillance, community intelligence, and commissioning decisions.
Three policy gaps stand out in high-income settings:
- Underserved-area mapping is weak: National plans often know prevalence patterns better than service-friction patterns.
- Community-led delivery remains underpowered: Formal systems still struggle to fund trust-based outreach at scale.
- Wraparound support is fragmented: Housing, migration status, stigma, and co-infection risks are often managed outside HIV planning.
A related discussion is worth watching here:
Syndemics expose institutional blind spots
The current challenge isn’t HIV in isolation. It is HIV as part of a wider syndemic environment that includes TB, hepatitis, substance use, insecure housing, incarceration, and migration-related exclusion. These overlaps punish administrative fragmentation. One agency funds testing, another funds treatment, another controls social support, and none owns the full pathway.
That’s where the absence of a UK national aids control council becomes analytically useful. It forces a sharper question than “which agency is in charge?” The question is whether any body has both the mandate and the political backing to connect epidemiology, community delivery, and cross-sector support in a single operating model.
A mature health system can still be structurally immature in the way it reaches people with the greatest barriers to care.
For G20 governments, the lesson is uncomfortable but clear. Advanced financing systems and complex surveillance do not compensate for weak delivery integration. If coordination bodies can’t reach migrants, homeless populations, and other underserved groups, the response remains incomplete no matter how strong headline policy looks.
Actionable Recommendations For G7 and G20 Policymakers
G7 and G20 governments shouldn’t ask whether they need to copy a foreign national aids control council. They should ask whether their current institutions perform the same high-value functions with equal clarity and authority. In many cases, they don’t.
Five practical steps follow from the comparative evidence:
Create or authorize one national coordinating authority. It doesn’t need the same name everywhere, but it does need clear responsibility for aligning HIV strategy, delivery, and accountability across ministries.
Use one results framework across the response. Prevention, treatment, retention, and community outreach should be measured in one system, not in parallel reporting channels that obscure trade-offs.
Treat community-led delivery as core infrastructure. Financing for peer networks, outreach, and navigation should be embedded in national plans, not treated as discretionary add-ons.
Budget for implementation quality. Workforce mentorship, certification, and frontline capability should be financed as core programme components, not secondary support functions.
Design HIV governance for syndemics, not silos. Coordination mechanisms should connect HIV to TB, hepatitis, homelessness, prison health, and migrant access rather than leave those issues to separate administrative tracks.
The strategic conclusion is simple. Countries that organise HIV policy as a narrow disease programme will keep rediscovering the same gaps in equity and retention. Countries that organise it as a statewide coordination challenge are better placed to protect gains, target need, and build governance machinery that also strengthens broader health security.
Global health governance works best when decision-makers learn across borders without copying blindly. For more analysis that translates international evidence into practical choices for ministers, multilaterals, and policy teams, visit Global Governance Media.